Former UF Health patient creates ‘coping kits’ for pediatric blood draws
Blood draws can be scary for young children. As they sit in the hospital chair, their heart rate speeds up as the nurse walks by. Anxiety rises as the needle…

Update your location to show providers, locations, and services closest to you.
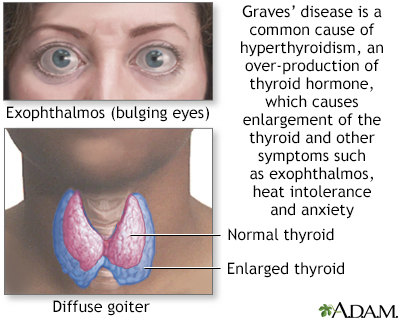
Graves disease is an autoimmune disorder that leads to an overactive thyroid gland (hyperthyroidism). An autoimmune disorder is a condition that occurs when the immune system mistakenly attacks healthy tissue.
Diffuse thyrotoxic goiter; Hyperthyroidism - Graves; Thyrotoxicosis - Graves; Exophthalmos - Graves; Ophthalmopathy - Graves; Exophthalmia - Graves; Exorbitism - Graves
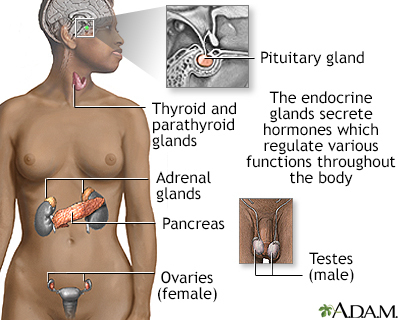
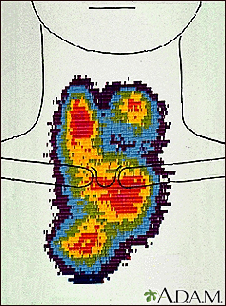
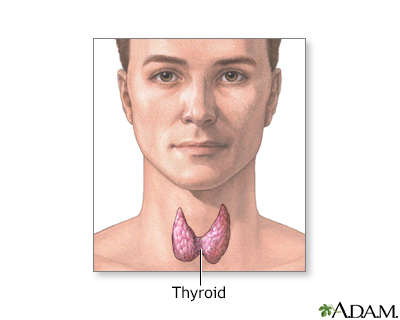
The thyroid gland is an important organ of the endocrine system. The gland is located at the front of the neck above where the collarbones meet. This gland releases the hormones thyroxine (T4) and triiodothyronine (T3), which control body metabolism. Controlling metabolism is important for regulating mood, weight, and mental and physical energy levels.
When the body makes too much thyroid hormone, the condition is called hyperthyroidism. (An underactive thyroid leads to hypothyroidism.)
Graves disease is the most common cause of hyperthyroidism. It is due to an abnormal immune system response that causes the thyroid gland to produce too much thyroid hormone. Graves disease is most common in women over age 20. But the disorder can occur at any age and can affect men as well.
Younger people may have these symptoms:
Many people with Graves disease have problems with their eyes:
Older people may have these symptoms:
During the physical exam, your health care provider may find:
Other tests include:
This disease may also affect the following test results:
Treatment is aimed at controlling your overactive thyroid. You may receive one or more types of treatment.
Beta-blocker medicines may help treat:
They may be given until the hyperthyroidism is controlled.
Antithyroid medicines:
Radioactive iodine is given by mouth. It then concentrates in the overactive thyroid tissue and causes damage.
Surgery may be done to remove the thyroid.
If you have had radioactive iodine treatment or surgery, you will need to take replacement thyroid hormones for the rest of your life. This is because these treatments destroy or remove the gland.
TREATMENT OF THE EYES
Some of the eye problems related to Graves disease often improve after treatment with medicines, radiation, or surgery. Radioiodine therapy can sometimes make eye problems worse. Eye problems are worse in people who smoke, even after the hyperthyroidism is treated.
Sometimes, prednisone is needed to reduce eye irritation and swelling. Prednisone is a steroid medicine that suppresses the immune system.
You may need to tape your eyes closed at night to prevent drying. Sunglasses and eye drops may reduce eye irritation. In rare cases, surgery or radiation therapy (different from radioactive iodine) may be needed to prevent further damage to the eye and loss of vision.
Graves disease often responds well to treatment. Thyroid surgery or radioactive iodine often will cause an underactive thyroid (hypothyroidism). Without getting the correct dosage of thyroid hormone replacement, hypothyroidism can lead to:
Call your provider if you have symptoms of Graves disease. Also call if your eye problems or other symptoms get worse or do not improve with treatment.
Go to the emergency room or call 911 or the local emergency number if you have symptoms of hyperthyroidism with:
Hollenberg A, Wiersinga WM. Hyperthyroid disorders. In: Melmed S, Auchus RJ, Golfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 12.
Jonklaas J, Cooper DS. Thyroid. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 213.
Marcdante KJ, Kleigman RM. Thyroid disease. In: Marcdante KJ, Kliegman RM, eds. Nelson Essentials of Pediatrics. 8th ed. Philadelphia, PA: Elsevier; 2019:chap 175.
Marino M, Vitti P, Chiovato L. Graves' disease. In: Jameson JL, De Groot LJ, de Kretser DM, et al, eds. Endocrinology: Adult and Pediatric. 7th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 82.
Ross DS, Burch HB, Cooper DS, et al. 2016 American Thyroid Association guidelines for diagnosis and management of hyperthyroidism and other causes of thyrotoxicosis. Thyroid. 2016;26(10):1343-1421. PMID: 27521067 pubmed.ncbi.nlm.nih.gov/27521067/.


Blood draws can be scary for young children. As they sit in the hospital chair, their heart rate speeds up as the nurse walks by. Anxiety rises as the needle…
